SEARCH:
FOLLOW ME:
SUBSCRIBE TO MY BLOG:
THE ACE STUDY
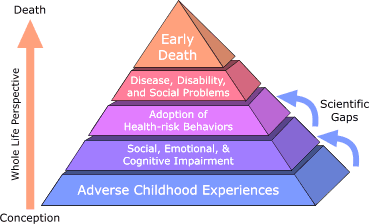
The Adverse Childhood Experiences (ACE) Study showed that for 17,337 patients, childhood trauma correlated to serious adult medical conditions. “Contrary to conventional belief," says co-Director Vincent Felitti, MD, "time does not heal all wounds, since humans convert traumatic emotional experiences in childhood into organic disease later in life.”FEATURED BOOKS – QUOTES
"Too many Americans are spurred to achieve, rather than to attach."
--A General Theory of Love "Trying to fix the heart using the head, is like trying to paint with a hammer - it only makes a mess."
"You can be strong - or you can be human." -- Grief Recovery Handbook "Gosh, I shoulda checked the milligramage! Oh, well, Live and Learn." -- Working Girl "Any book you haven't thrown across the room at least once because it smashed your world view, probably isn't worth a long shelf life." -- Kathy "Mental health. For everything else there's MasterCard." -- Kathy-
RECENT POSTS
- Singing for Joy after Trauma: My Music Video! May 17, 2018
- Parenting as We Were Parented May 10, 2018
- I had a blast: “Mary Giuliani LIVE!” Apr 18 April 17, 2018
- My Book’s Amazon Reviews: Music & Healing April 3, 2018
- Six-City Bus Tour: Campaign to Heal Childhood Trauma March 23, 2018
RECENT COMMENTS
- Paula Kinghorn on Featured Topics
- Saria bushmire on Find a Support Group
- whoiscall on Singing for Joy after Trauma: My Music Video!
- deen on Blogs
- Lin Rhodes on Featured Topics
ARCHIVES
Tag Archives: attachment disorder
Six-City Bus Tour: Campaign to Heal Childhood Trauma
Join me and my friends at Calo Programs, Attachment and Trauma Network (ATN), the American Adoption Congress (AAC) and the Association for Training on Trauma and Attachment in Children (ATTACh) for their “Campaign to Heal Childhood Trauma.” It’s a six-city … Continue reading →
5,112 total views
Posted in Attachment, Attachment Disorder, Attachment Theory, Brain Science, Emotional pain, Fight-Flight, Trauma
|
Tagged ACE Study, American Adoption Congress (AAC), ATTACh, Attachment and Trauma Network (ATN), attachment disorder, Attachment Disorder Healing, Calo Programs, Campaign to Heal Childhood Trauma, Developmental Trauma, Mental Health, Trauma-Informed Care
|
Leave a comment
Pediatricians Screen for Child Trauma
“To prevent childhood trauma, pediatricians screen children and their parents…and sometimes, just parents…for childhood trauma” — guest blog by Jane Ellen Stevens, Editor, ACEsTooHigh.com and ACEsConnection.com When parents bring their four-month-olds to a well-baby checkup at the Children’s Clinic in Portland, … Continue reading →
5,844 total views
Excommunication Blues
#16 in my book blogs from “Don’t Try This at Home,” Chapter 3 Last time, I wrote that just when I thought 2008 couldn’t get any worse, October-November 2008 with Mom in the hospice in Florida turned out to be … Continue reading →
9,494 total views
Posted in Attachment, Attachment Disorder, Attachment Theory, Brain Science, Dissociation, Emotional pain
|
Tagged Adult Attachment Disorder, Adult Attachment Interview, Adult Attachment Theory, attachment disorder, brain science, Brain stem, Dissociation, Emotional pain, Need-Fear Dilemma, therapy, Ugly Duckling
|
2 Comments
I Oughtta Have My Head…
#11 in my ongoing book blogs from “Don’t Try This at Home” After my divorce and the saga with Rebound Dan back East, did I mention dating in California? I did meet several fellows who looked promising at first. Harvey … Continue reading →
8,515 total views
Posted in Attachment, Attachment Disorder, Brain Science, Divorce, Emotional pain, Grief
|
Tagged Attachment, attachment disorder, brain science, codependent, Divorce, Emotional pain, Grief, Limbic brain, post-divorce dating, PTSD, rebound, repetition compulsion, therapy, trauma
|
7 Comments
Tin Can Shot Full of Holes
#10 in my ongoing book blogs from “Don’t Try This at Home” After my Dad’s funeral, back I flew from Florida again to my consulting gig near Washington DC, and to Dan the rebound affair, who seemed supportive. I was … Continue reading →
5,451 total views
When Family Doesn’t Get It, Recovery Partners Will
#4 in the news blog series; original post on ACEsConnection, September 26, 2013 When we’re hurting, we all want and need those closest to us to “get it,” but please take comfort from the statistic that it usually does not … Continue reading →
6,224 total views
Posted in Attachment Disorder, Attachment Theory, Emotional pain, Grief, Trauma
|
Tagged Al Anon, attachment disorder, DivorceCare, Emotional pain, Grief, Grief Recovery Handbook, Jack Kornfield, John James, John Townsend, Matthew Warren, Rick Warren, Russell Friedman, Suicide, trauma
|
Leave a comment
No Tears for Dad
#9 in my ongoing book series; original post September 27, 2013 After my 27-year marriage fell apart, by late 2007 I was reduced to writing long poems for Dan the East Coast rebound affair, in a bizarre attempt to figure … Continue reading →
3,289 total views
Enter the Dragon
#8 in my ongoing book series; original post September 20, 2013 OK, step away from the brain science; back to how my life fell apart with Attachment Disorder. When we last looked at the end of my 27-year marriage, I’d … Continue reading →
6,089 total views
Posted in Attachment, Attachment Disorder, Brain Science, Divorce, Emotional pain, Grief
|
Tagged affair, Attachment, attachment disorder, brain science, Bruce Lee, Bruce Perry, Come Here Go Away, Divorce, Emotional pain, Enter the Dragon, Grief, Helen Fisher, Limbic brain, rebound, Stephen Porges
|
2 Comments
How Your Brain Works 101
CLICK to BUY “Don’t Try This Alone” Dr. Bruce Perry just put out his latest on “How Your Brain Works 101,” in a September 5 webinar for the National Council on Behavioral Health. Perry’s revelations at Dr. Daniel Siegel’s March … Continue reading →
46,751 total views
Posted in Attachment, Attachment Disorder, Attachment Theory, Brain Science, Dissociation, Emotional pain, Trauma
|
Tagged Attachment, attachment disorder, Attachment Theory, brain science, Bruce Perry, Daniel Siegel, Developmental Trauma, Dissociation, Emotional pain, Henry Cloud, Limbic brain, Peter Levine, trauma
|
15 Comments
Surgeon General’s Warning: Rebound!
#7 in my ongoing book series; original post September 6, 2013 I never liked the sticky suburbs of Washington D.C. My ex had moved us there from New York City years before. As I was boxing up my three-bedroom Virginia … Continue reading →
6,104 total views
Posted in Attachment, Attachment Disorder, Dissociation, Divorce, Emotional pain, Grief
|
Tagged affair, Attachment, attachment disorder, Disorder, Dissociation, Divorce, Emotional pain, Grief, rebound, Toby Keith, Wilma Flintstone
|
2 Comments

